Medicaid, established in 1965 under the Social Security Amendments, is a vital program within the United States healthcare system. It serves as a government-sponsored health insurance initiative aimed at providing medical assistance to low-income individuals and families, including children, the elderly, and people with disabilities. Over the decades, Medicaid has grown to become one of the largest sources of health coverage in the United States, covering more than 83 million people as of 2023. This article explores the structure, impact, challenges, and future of Medicaid, shedding light on its crucial role in American society.
1. Origins and Development of Medicaid
Medicaid was created as part of President Lyndon B. Johnson’s “Great Society” programs, designed to reduce poverty and racial injustice. The program was conceived alongside Medicare, which primarily serves older Americans, to address the healthcare needs of low-income individuals. Initially, Medicaid coverage was limited, focusing mainly on individuals receiving cash assistance. However, it quickly expanded to include a broader array of people in need, such as children, pregnant women, the elderly, and people with disabilities.
Over the years, federal and state governments have collaborated to shape Medicaid, which is jointly funded by both. The federal government provides a baseline of financial support, while states administer the program and tailor it to their residents’ specific needs, resulting in variations across states in terms of eligibility, benefits, and coverage.
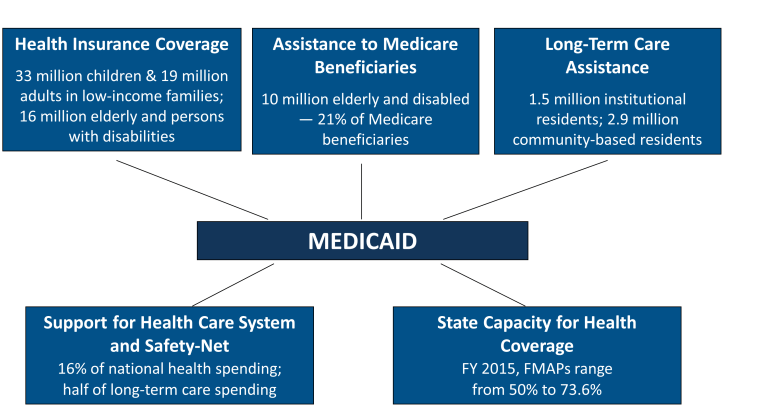
2. Structure and Funding of Medicaid
Medicaid operates under a federal-state partnership. While the federal government establishes broad guidelines, states have significant discretion in how they implement the program. This flexibility allows states to adapt their Medicaid programs to local conditions, but it also leads to variability in coverage and services across the country.
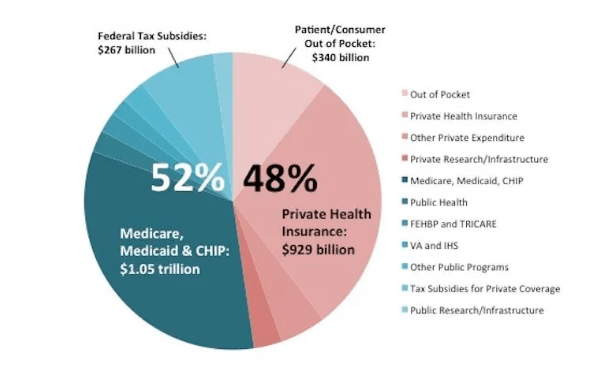
Funding: Medicaid funding is derived from both federal and state sources. The federal government contributes a percentage of each state’s Medicaid costs through the Federal Medical Assistance Percentage (FMAP), which varies based on the state’s per capita income. In wealthier states, the federal contribution might be as low as 50%, while in poorer states, it can be as high as 77%. States are responsible for covering the remaining costs. The Affordable Care Act (ACA) of 2010 introduced an expansion of Medicaid, offering states additional federal funds to cover low-income adults without children, which many states have adopted.
Eligibility: Medicaid eligibility is determined by a combination of federal and state criteria. Generally, it covers low-income families, pregnant women, elderly adults, and people with disabilities. The ACA’s Medicaid expansion aimed to extend coverage to all adults with incomes up to 138% of the federal poverty level, though this expansion was made optional for states by a 2012 Supreme Court decision. As of 2023, 39 states and the District of Columbia have adopted Medicaid expansion, resulting in significant increases in coverage.
Benefits: Medicaid provides a wide range of health services, including hospital care, physician services, long-term care, and preventive services. Mandatory benefits set by the federal government include inpatient and outpatient hospital services, laboratory and X-ray services, and nursing facility services for adults. States may also offer optional benefits such as prescription drugs, dental care, and physical therapy, leading to variability in services across the country.
3. Impact of Medicaid on Health Outcomes and Society
Medicaid has had a profound impact on the health and well-being of millions of Americans. Its reach is broad, covering one in five Americans, and it plays a particularly critical role for vulnerable populations. Here are some key ways in which Medicaid has impacted health outcomes and society:
Access to Care: Medicaid significantly improves access to healthcare for low-income individuals. Studies have shown that Medicaid recipients are more likely to have a regular source of care, receive preventive services, and access necessary medical treatment compared to uninsured individuals. This access to care helps prevent the worsening of health conditions, reducing the need for emergency care and hospitalizations.
Health Outcomes: The availability of Medicaid has been associated with better health outcomes, particularly for children and pregnant women. For instance, children with Medicaid coverage are more likely to receive vaccinations and preventive care, leading to lower rates of chronic conditions. Pregnant women on Medicaid have better access to prenatal care, which contributes to healthier pregnancies and better birth outcomes.
Financial Protection: Medicaid provides critical financial protection for low-income families. Without Medicaid, many families would face significant medical debt and financial hardship. Medicaid helps to alleviate the burden of medical costs, ensuring that families can access necessary healthcare services without the fear of financial ruin.
Economic Impact: Beyond individual health outcomes, Medicaid also has broader economic implications. By providing health coverage, Medicaid enables low-income individuals to seek employment and maintain their health, contributing to the workforce. Additionally, Medicaid funding supports healthcare providers, particularly in underserved areas, ensuring the viability of hospitals and clinics that serve low-income communities.
4. Challenges Facing Medicaid
Despite its successes, Medicaid faces several challenges that impact its effectiveness and sustainability:
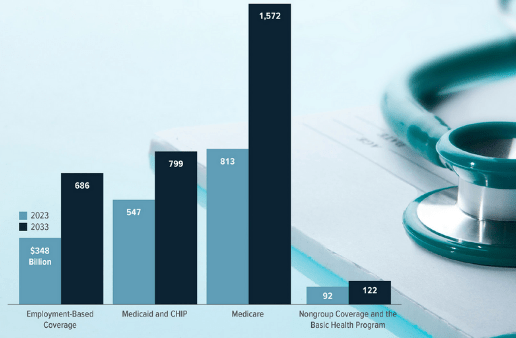
Funding Pressures: As healthcare costs continue to rise, Medicaid’s funding structure faces increasing pressure. States must balance their budgets while covering their share of Medicaid costs, which can be challenging during economic downturns. Moreover, as the aging population grows, the demand for Medicaid’s long-term care services is expected to increase, further straining resources.
Variability Across States: The flexibility granted to states in administering Medicaid results in significant variability in coverage, benefits, and access to care. This variability can lead to disparities in health outcomes and access to services, depending on where individuals live. States with more generous Medicaid programs tend to have better health outcomes, while states with limited coverage face higher rates of uninsured individuals.
Provider Participation: Medicaid reimbursement rates are often lower than those of private insurance and Medicare, which can discourage healthcare providers from participating in the program. This can lead to limited access to care for Medicaid recipients, particularly in rural and underserved areas where there may be fewer providers willing to accept Medicaid patients.
Political and Policy Challenges: Medicaid is frequently at the center of political debates, with differing views on its role, funding, and scope. Changes in administration and shifts in political priorities can lead to uncertainty and instability in Medicaid policy, affecting beneficiaries, providers, and state budgets.
5. The Future of Medicaid
The future of Medicaid will likely be shaped by ongoing policy debates, demographic changes, and healthcare needs. Key considerations for the future include:
Medicaid Expansion: As of 2023, several states have yet to adopt Medicaid expansion under the ACA. Ongoing efforts to encourage expansion could increase coverage and reduce the number of uninsured individuals, particularly in states with high rates of poverty and health disparities.
Integration with Other Health Programs: To improve care coordination and outcomes, there is a growing emphasis on integrating Medicaid with other health and social service programs. This includes better coordination with Medicare for individuals eligible for both programs and integration with programs addressing social determinants of health, such as housing and nutrition.
Innovative Payment Models: To address rising healthcare costs and improve quality, there is a push towards value-based payment models within Medicaid. These models aim to incentivize healthcare providers to deliver high-quality, cost-effective care, focusing on outcomes rather than volume of services.
Addressing Health Disparities: Medicaid has the potential to play a significant role in reducing health disparities by improving access to care for marginalized communities. Targeted efforts to address social determinants of health and expand access to preventive services can help reduce disparities and improve health equity.
Long-Term Care: With an aging population, the demand for long-term care services is expected to grow. Medicaid is the largest payer for long-term care in the United States, and future policies will need to address the sustainability and adequacy of these services to meet the needs of elderly and disabled individuals.
Conclusion
Medicaid is a cornerstone of the American healthcare system, providing essential health coverage to millions of low-income individuals and families. Its impact on health outcomes, access to care, and financial protection is undeniable. However, Medicaid faces significant challenges that must be addressed to ensure its sustainability and effectiveness. As the United States continues to grapple with healthcare reform, the role of Medicaid will remain crucial in promoting the health and well-being of vulnerable populations and achieving a more equitable healthcare system. The future of Medicaid will depend on continued innovation, collaboration, and commitment to addressing the healthcare needs of all Americans.










mizon5
vlq01p